

Indian Journal of Science and Technology
Year: 2020, Volume: 13, Issue: 29, Pages: 3002-3007
Original Article
Nisa Aulia Paramitha1*, Udadi Sadhana2, Awal Prasetyo2, Vega Karlowee2
1Undergraduate Student, Faculty of Medicine, Diponegoro University, Semarang, Indonesia
2Lecturer, Department of Pathology Anatomy, Faculty of Medicine, Diponegoro University,Semarang, Indonesia
*Corresponding Author
Email: [email protected]
Received Date:21 April 2020, Accepted Date:10 June 2020, Published Date:11 August 2020
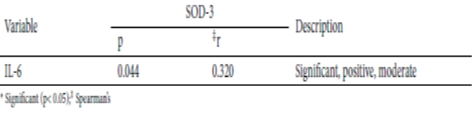
Background: Occupational air pollution exposure in textiles industry which irritates the respiration system triggers the disturbance of the nasal mucosa.IL-6 is produced by monocytes and macrophages as a response for tissue damage. SOD-3 is extracellular enzymes protected the tissue from free radical and chronic inflammation. Objectives: To know if the occupational air pollution affects the increasing of IL-6 and SOD-3 level on nasal wash. Methods: this study used an analytical observational design with cross-sectional method. It was conducted on 40 male workers of garment industry in Bawen, Semarang,Indonesia. Divided into two groups: the dyeing and sizing area with 20 workers each group. The workers exposed to the occupational air pollutant for 5 years or more. The aquabidest will be injected to subject’s nosetril using the 20cc spuit. The nasal wash’s sample on the 1.5ml eppendorf tubes will be examined using ELISA method to determine the IL-6 and SOD-3 level. The occupational air pollution indicators will be measured by Envilab Semarang. Findings : The measurements of direct PM10 and PM2.5 in dyeing and sizing area were higher than the regulatory limit. There was a significant difference in the IL-6 level in dyeing and sizing area (p=0,010). There was no significant difference in the SOD-3 level in dyeing and sizing area (p=0,443). There was a positive, moderate and significant correlation between IL-6 and SOD-3 in dyeing and sizing area (r=0.320). Conclusion: The study concluded that the occupational air pollution especially the PM10 and PM2.5 affects the IL-6 and SOD-3 level in the textile industry workers’ nasal wash. There is a significant correlation between the IL-6 and SOD-3 level in textile industry workers at dyeing and sizing area. There is a difference in the IL-6 level in dyeing and sizing area. But there is no significant in the SOD-3 level in dyeing and sizing area. The higher occupational air pollution inhaled will be compensated with the higher expression of IL-6 and SOD-3. The higher exposure of PM2.5 in the dyeing area results in the higher level of IL-6 and SOD-3.
Keywords: Interleukin 6; superoxide dismutase 3; occupational air pollution;ELISA
© 2020 Paramitha et al.This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Published By Indian Society for Education and Environment (iSee).
Subscribe now for latest articles and news.